ADHD and Nutrition for Athletes: Why Your Brain Needs a Different Fuelling Strategy
You've done your research. You know you should increase your protein intake, schedule your carbs around workouts, and prepare meals on Sundays. Nevertheless, it's Tuesday evening. You missed breakfast because medication suppressed your appetite, trained on an empty stomach at lunchtime, and now you're in the kitchen at 9pm, eating cereal straight from the box. Again.
If that sounds familiar, it's not because you lack discipline. It's because most nutrition advice for athletes was designed for a neurotypical brain — one that can plan ahead, remember to eat, and follow through without scaffolding. If you have ADHD, that advice was never designed for you. This post reframes nutrition as a training variable, not a test of willpower, and offers a fuelling approach tailored to how the ADHD brain actually works.
Table of Contents:
Why ADHD Athletes Need a Different Fuelling Strategy
The Medication-Appetite Trap
The Dopamine-Food Cycle: Why Your Brain Craves the Wrong Fuel at the Wrong Time
Why Every Nutrition Plan Fails the ADHD Athlete
Building an ADHD-Compatible Fueling System
What the Science Says: Nutrients that Matter for the ADHD Athlete
Conclusion
Why ADHD Athletes Need a Different Fuelling Strategy
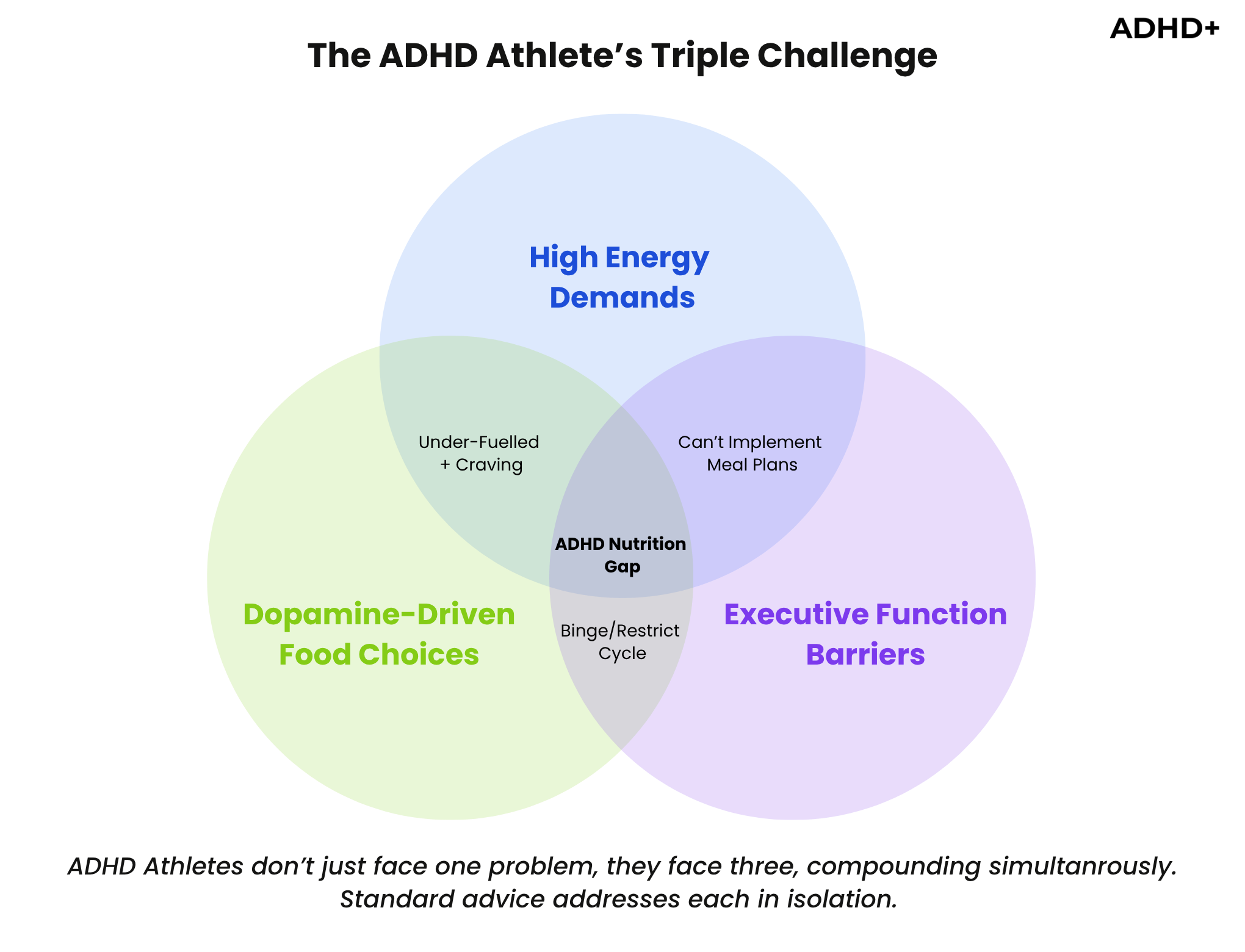
ADHD doesn't just affect your focus during training. It changes how your brain and body process, seek, and use fuel — and those differences are intensified by the physical demands of sport.
The energy gap most athletes don't know about
Here's something most ADHD athletes have never been told: your body likely burns more energy at rest than a neurotypical athlete's. Research published in the journal Nutrients in January 2026 found that children with ADHD who are not on medication have a resting energy expenditure approximately 6.5 kilocalories per kilogram of fat-free mass higher than those without ADHD, which translates to roughly 325 extra calories per day for a 50kg athlete (Solgard et al., 2026). Layer training demands on top of that baseline deficit, and you begin to understand why so many ADHD athletes feel chronically under-fuelled without knowing why.
Interestingly, the same research found that ADHD athletes who are on stimulant medication show the opposite pattern, lower overall physical activity expenditure during medicated hours, which changes the energy equation again depending on whether you train while medicated or not (Sogard et al., 2026).
It’s not about what you eat, it’s about what your brain lets you do
The internet is full of articles telling you which foods to eat for ADHD. Protein for dopamine. Omega-3s for focus. Complex carbs for sustained energy. That information isn't wrong, but it misses the point.
The real challenge for ADHD athletes isn't knowing which nutrients matter. It's building the executive function infrastructure that makes consistent fuelling possible. Planning meals, shopping for ingredients, remembering to eat during a busy training day, and resisting impulses when you're depleted are all executive function tasks. And executive function is precisely what ADHD impairs.
This is where the conversation needs to shift from dietetics to coaching. The science of what to eat is well established. The system of how to eat consistently, with an ADHD brain, in the context of athletic training — that's the piece almost nobody is talking about.
The Medication-Appetite Trap
If you take stimulant medication for your ADHD, methylphenidate (Concerta, Ritalin) or amphetamine-based drugs (Adderall, Vyvanse, Elvanse), you already know the deal. The medication helps with your focus and concentration. It also suppresses your appetite, sometimes to the point where food becomes genuinely unappealing.
Research confirms that this is one of the most common and persistent side effects of stimulant treatment. Stimulants increase dopamine and norepinephrine levels in the brain, which may blunt hunger cues, reducing the motivational drive for food; effectively suppressing appetite even when the body needs fuel (Bail, 2021; Wellman, 2005). For athletes, this creates a specific and predictable problem.
The timeline that works against you
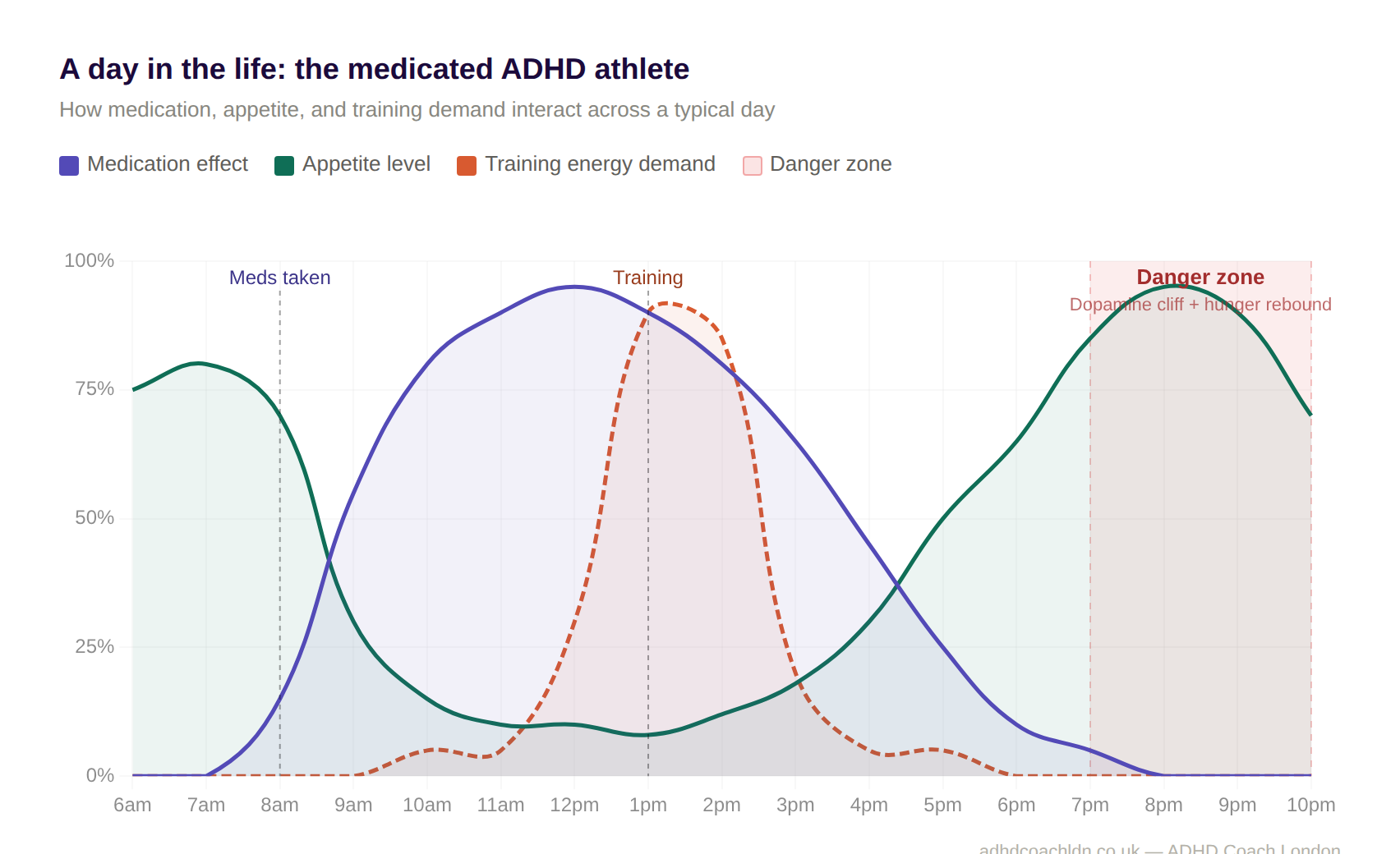
Walk through a typical day for a medicated ADHD athlete:
7:00–8:00 am — Medication taken. Maybe you eat something first, maybe you don't.
9:00 am — Appetite disappears. You're focused, productive, not thinking about food.
12:00–2:00 pm — Training session. Your body needs fuel. Your brain says you're fine.
3:00–5:00 pm — Medication at peak. You've now been active on minimal calories for hours.
6:00–7:00 pm — Medication wears off. Hunger hits like a wall.
8:00–10:00 pm — Overconsumption. Quick-dopamine foods. Peanut butter from the jar. The cereal box. Whatever requires zero executive function to prepare.
This isn't a willpower failure. It's a pharmacological pattern — and it's entirely coachable once you recognise it.
Sports nutritionist Nancy Clark, writing for the American College of Sports Medicine, recommends that athletes with ADHD eat a substantial breakfast before their medication takes effect, then fuel by the clock rather than by hunger cues — eating at scheduled intervals regardless of appetite (Clark, 2022/2025). She suggests reframing "snack" as "second lunch" to encourage higher-quality food choices and using calorie-dense liquids, such as protein shakes, when solid food feels impossible (Clark, 2022/2025).
This is sound advice. But it still assumes you'll remember to set the alarm, prepare the food in advance, and follow through when every fibre of your being says, "I'm not hungry." That's where coaching, external accountability, environmental design, and ADHD-specific implementation strategies become the missing link.
What does this look like in practice
From my coaching work, I see this pattern constantly. Clients describe knowing they need to eat but feeling physically unable to; the food tastes like nothing; the act of chewing feels like a chore; and the executive energy required to prepare even a simple meal feels disproportionate to the reward. By evening, the dam breaks. The hunger is real, the dopamine-seeking is intense, and the food choices reflect that urgency.
The goal isn't to eliminate this pattern entirely; medication may always affect appetite. The goal is to build a system that minimises the damage during the suppressed window and manages the rebound intelligently.
The Dopamine-Food Cycle: Why Your Brain Craves the Wrong Fuel at the Wrong Time
ADHD brains have lower baseline levels of dopamine, the neurotransmitter that drives motivation, reward, and pleasure (ADDitude Magazine; Sogard et al., 2026). This is one of the reasons stimulant medications work: they increase dopamine availability, which improves focus and reduces impulsivity.
But dopamine doesn't just come from medication. It also comes from exercise and from food, particularly sugar, salt, and hyperpalatable processed food. For athletes with ADHD, these three dopamine sources interact in ways that create predictable vulnerability windows.
The post-training dopamine cliff
During training, your brain gets a significant dopamine boost from physical activity. If you're also medicated, you have a second source of dopamine that supports your focus and drive. This is often when ADHD athletes feel at their best; locked in, energised, performing.
The problem comes when training ends.
If your medication wears off around the same time as your training session finishes, which, for afternoon or evening trainers, it often does, you experience a double dopamine withdrawal. The exercise-driven boost fades. The medication-driven boost fades. And your already dopamine-deficient brain is suddenly running on empty.
What does a dopamine-depleted brain do? It seeks the fastest available source of reward. And the fastest available source, when you're exhausted and standing in your kitchen, is almost always food. Not a carefully prepared chicken breast with quinoa. Crisps. Biscuits. Toast with Nutella. Whatever is immediate requires no preparation and delivers a sensory hit.
This isn't emotional eating. It's neurochemical. Your brain is doing exactly what it's wired to do.
Working with dopamine, not against it
The coaching approach here isn't to fight the craving; that's an executive function that your depleted brain can't reliably sustain at 8 pm after a hard session. Instead, the approach is to design your environment so that when the dopamine cliff hits, the path of least resistance is still a reasonable fuelling choice.
What this looks like practically:
Pre-prepare a post-training meal before you leave for your session. When you return depleted, the meal is ready. No decisions required. No cooking. Just eat. This is easier to do when your medication is still active, and your executive function is higher.
Use the "dopamine bridge." A small, intensely satisfying snack immediately after training, such as a handful of salted nuts, dark chocolate, or a protein bar with a flavour you actually enjoy, to take the edge off the craving while your proper meal heats up. The bridge stops you from eating everything in the cupboard before your real food is ready.
Lean into umami and texture. Dopamine-seeking brains respond to flavour intensity and texture variety. Build post-training meals around strong flavours such as soy sauce, chilli, garlic, smoked foods, and crunchy toppings on soft bases. This satisfies the neurological craving without resorting to sugar.
Stop moralising food. Fracturing foods into "good" and "bad" creates shame spirals that are uniquely destructive for ADHD brains. The goal is adequate fuelling with enough variety to sustain interest, not nutritional perfection.
Why Every Nutrition Plan Fails the ADHD Athlete
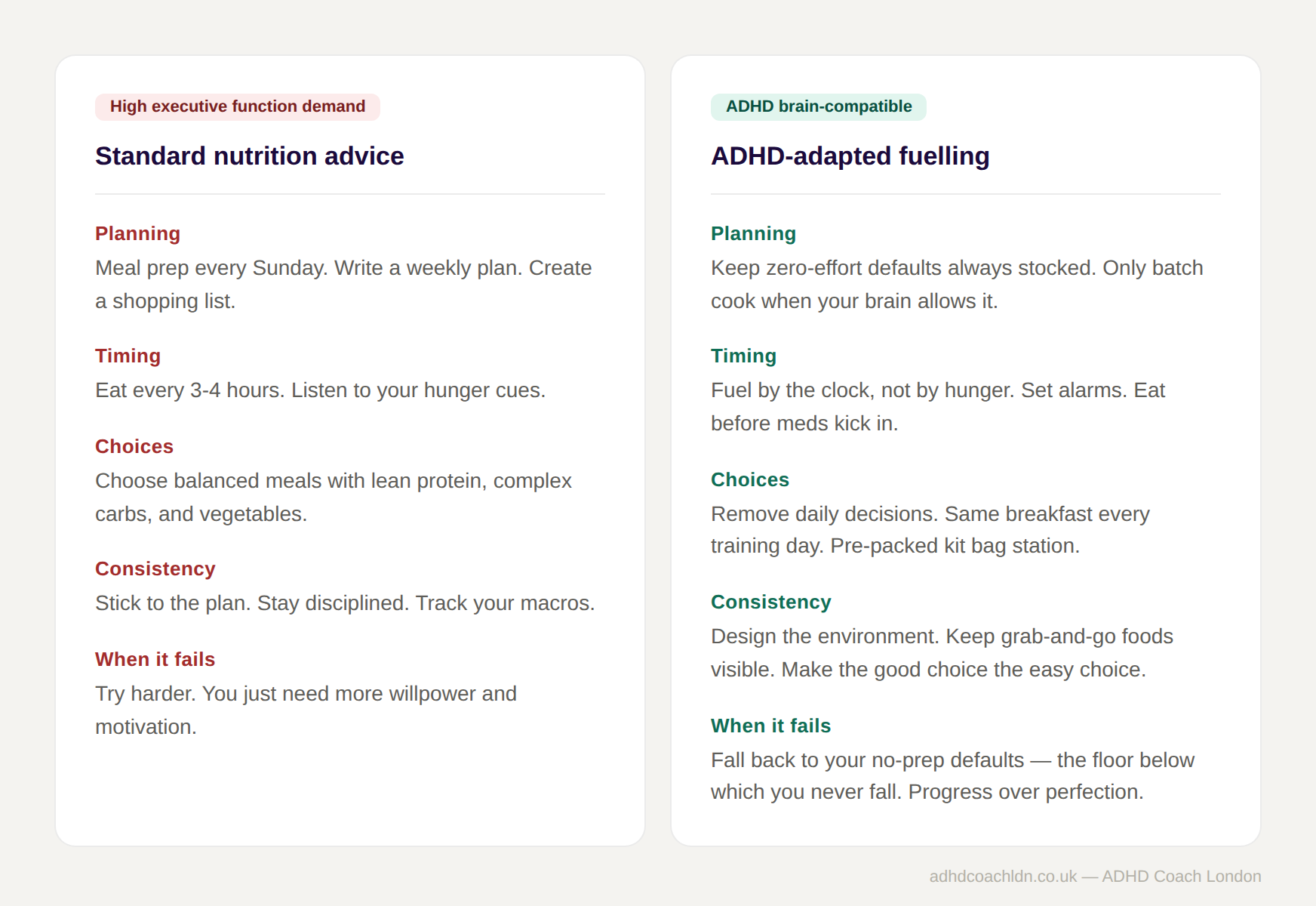
Every article on ADHD nutrition on the internet will tell you to meal prep, plan ahead, eat on a schedule, and stock your fridge with healthy options. The advice is clinically sound. It also assumes the very cognitive capacities that ADHD impairs.
The executive function gap in nutrition advice
Think about what "meal prep on Sunday" actually requires: anticipating what you'll want to eat over the coming week (planning), creating a shopping list (organisation), going to the shop and buying the right items (task initiation and working memory), spending 1-2 hours cooking (sustained attention), portioning and storing meals (follow-through), and remembering to take the meal with you when you leave the house (prospective memory).
That's six distinct executive functions in a single task. For a neurotypical brain, this is manageable. For an ADHD brain, particularly one that's unmedicated on a Sunday or fatigued after a week of training, it's a mountain to climb.
The predictable result? You do it perfectly for one week. Maybe two. Then executive function dips during a stressful period, a competition, or a disrupted routine, and the whole system collapses. You go from immaculate meal prep to takeaway every night, with nothing in between.
The all-or-nothing pattern
This binary pattern, perfect or nothing, is one of the most common ADHD experiences across all domains, not just in nutrition. Each cycle of collapse generates shame, which erodes motivation and makes the next attempt even harder to initiate.
The coaching reframe is this: stop optimising for the best-case scenario and start designing for the worst case. The question isn't "what's the ideal nutrition plan?" It's "what's the minimum viable fuelling strategy that keeps me adequately fed even on my worst executive-function day?"
Building an ADHD-Compatible Fuelling System
Here's where we move from diagnosis to action. If standard meal plans require too much executive function, the alternative isn't to give up on nutrition; it's to build a fuelling system with fewer cognitive demands and greater environmental support.
Periodise your nutrition like you periodise your training
Athletes don't train at the same intensity every day. You have heavy sessions and recovery days, competition blocks and off-season periods. Your nutrition system should reflect the same variability, specifically, the variability of your executive function.
Some days, your brain is firing. You've slept well, your medication is working, and you feel capable. Those are the days to batch-cook, try new recipes, and stock up. Other days, you're running on fumes, your focus is shot, and making a sandwich feels like project management. Those are the days when your system needs to catch you.
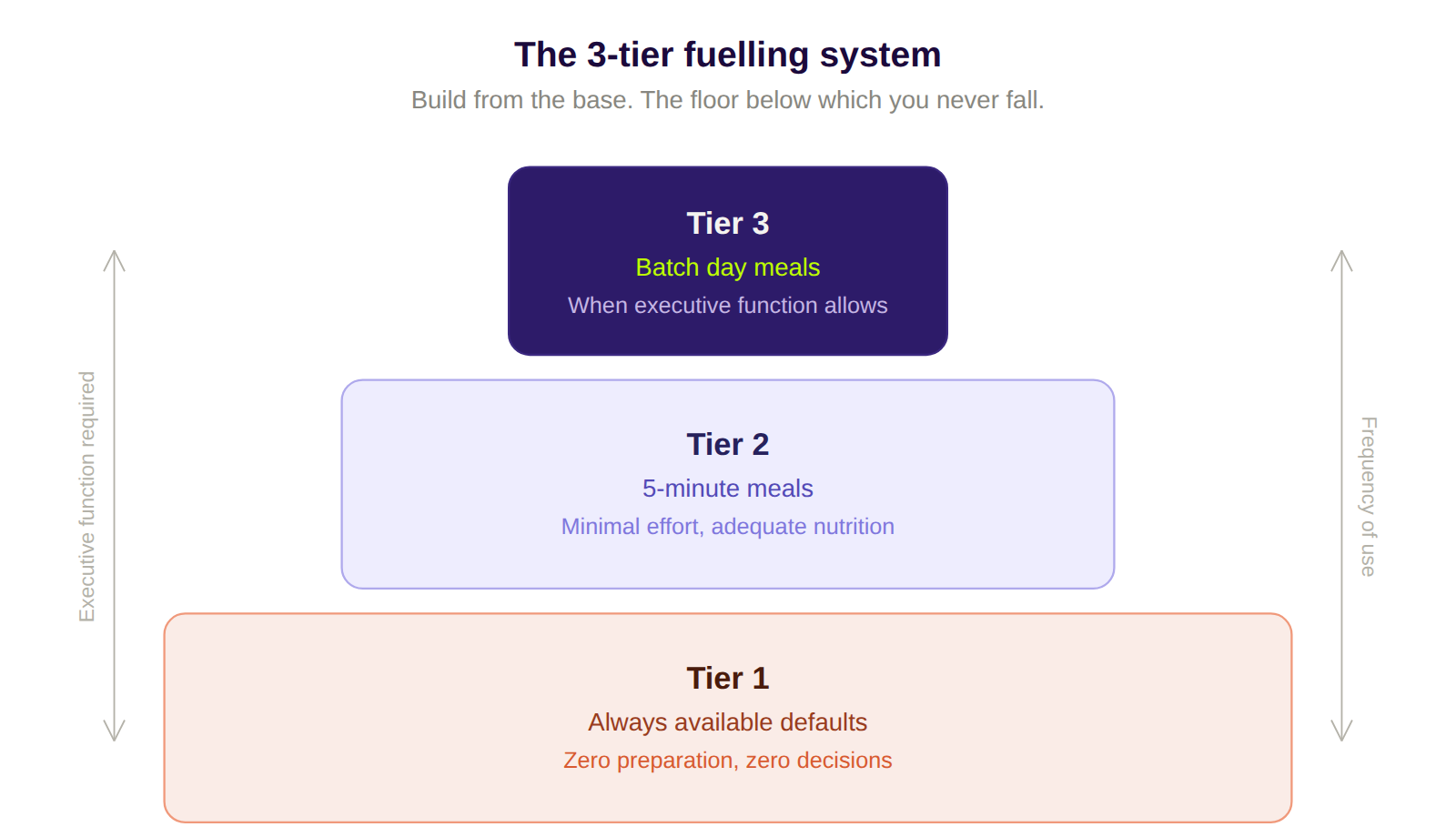
The framework I use with clients is a three-tier fuelling system:
Tier 1: "Always Available" Defaults (zero preparation, zero decisions). These are the foods that require nothing from you. They live in your cupboard, your gym bag, your desk drawer. They are your non-negotiable baseline, the floor below which you never fall.
Examples: pre-portioned nuts and seeds, protein shakes (buy ready-made, not powder that needs blending), bananas, tinned fish, pre-cooked rice pots, oat bars, peanut butter sachets, boiled eggs (batch-boiled and kept in the fridge).
Tier 2: "5-Minute Meals" (minimal effort, adequate nutrition). These are simple combinations that require minimal assembly but no real cooking. Your standard for average days.
Examples: eggs scrambled with spinach on toast, Greek yoghurt with fruit and seeds, a wrap with tinned tuna and pre-washed salad, overnight oats (prepared in 2 minutes the night before), a bowl of leftovers reheated from a Tier 3 day.
Tier 3: "Batch Day" Meals (proper cooking, done when executive function allows). These happen when you feel motivated, and only then. The key is to cook in volume and freeze in single portions, so one hour of effort generates 5-8 meals you can deploy on Tier 1 and Tier 2 days.
Examples: a big pot of chilli, a curry with rice, a stir-fry portioned into containers, a tray of roasted chicken and vegetables. Anything that reheats well and freezes without losing its appeal.
The system works because it removes the daily decision. You don't ask "what should I eat today?" You ask, "What tier am I operating at today?", and the answer is usually obvious within 30 seconds of waking up.
Environmental design over willpower
The second coaching principle: don't rely on your ADHD brain to make good decisions in the moment. Design your environment so the good decision is the default.
Keep Tier 1 foods visible and within reach. Not in the back of a cupboard. On the counter. In front of the fridge. In your gym bag. Out of sight is out of mind, and ADHD brains are especially susceptible to this.
Eliminate decision fatigue at breakfast. Eat the same thing every training day. This sounds boring, but it removes the single biggest friction point of the day. Save your decision-making energy for what actually matters.
Set up a "fuelling station" in your kit bag. Include a protein bar, a banana, a small bag of nuts, and a pre-made shake. This is your Tier 1 mobile unit. It goes with you to every session. It takes 2 minutes to assemble on a Sunday and eliminates the post-training crisis all week.
Use a visual system, not a written plan. ADHD brains respond better to visual cues than to text-based instructions. A whiteboard on the fridge with three meal options for the day, a colour-coded calendar, or even a photo of your pre-prepared meal — these outperform a detailed meal plan that lives in a note app you'll never open.
The role of accountability
Let me be clear: external accountability isn't a sign of weakness; it's a valuable performance tool. Just as elite athletes rely on coaches for technique, conditioning, tactics, and mental preparation, athletes with ADHD benefit from guidance tailored to the executive function challenges of daily life, including nutrition. This can be a coach, a nutritionist familiar with ADHD, a training partner checking your fuelling, or a structured program.
Having external accountability eases the burden on your executive functions and boosts the chances of following through. This is a well-documented finding in ADHD coaching research, and I see it confirmed weekly in my own practice.
Tier 1 is your non-negotiable baseline: nuts, protein shakes, bananas, tinned fish. Tier 2 is your average day: eggs on toast, yoghurt with fruit, and a wrap. Tier 3 happens when your brain allows it: curry, chilli, stir-fry in bulk.
What the Science Says: Nutrients That Matter for the ADHD Athlete
The fueling system above is central, but understanding which nutrients should take precedence is helpful. Here's a concise, evidence-based overview, not comprehensive but covering the most well-supported research.
Protein and tyrosine-rich foods are the building blocks for dopamine and norepinephrine, the neurotransmitters most implicated in ADHD. Starting the day with protein (eggs, Greek yoghurt, nuts, lean meat) before your medication kicks in gives your brain the raw materials for neurotransmitter production and helps stabilise blood sugar through the morning (ADDitude Magazine, 2025; Clark, 2022/2025).
Omega-3 fatty acids (EPA and DHA) have the strongest evidence base of any nutritional intervention for ADHD. Multiple reviews have found that people with ADHD tend to have lower omega-3 levels and that supplementation can produce modest improvements in attention and reduce impulsivity (Pelsser et al., 2023). For athletes, omega-3s also support recovery and help manage exercise-induced inflammation. Oily fish (salmon, mackerel, sardines) twice a week is the dietary target.
Iron is worth specific attention. Iron deficiency is common in both ADHD populations and in athletes, particularly female athletes, and the symptoms of iron deficiency (fatigue, poor concentration, impulsivity, disrupted sleep) directly overlap with ADHD symptoms, making it easy to attribute iron-related problems to ADHD alone (Sogard et al., 2026; Pelsser et al., 2023). A blood test to measure ferritin levels is a straightforward and valuable step. Severe iron deficiency has been associated with a 30% increase in impulsive and inattentive behaviours (adhd.clinic, 2025).
Magnesium supports hundreds of metabolic processes, including muscle recovery, sleep quality, and nervous system regulation. Research has found negative correlations between magnesium levels and ADHD symptom severity, meaning lower magnesium is associated with more pronounced symptoms (Sheridan et al., 2025). For athletes, magnesium also supports lactate clearance and vitamin D absorption. Good dietary sources include leafy greens, nuts, seeds, and whole grains.
Complex carbohydrates provide sustained glucose, the brain's primary energy source. For ADHD athletes, sustained-release carbs matter more than the type: whole grains, sweet potatoes, oats, and legumes deliver steady fuel without the spike-and-crash pattern that simple sugars create. Pairing carbohydrates with protein at every meal helps maintain stable blood sugar and supports both cognitive and physical performance (Clark, ACSM; Sogard et al., 2026).
An important note: The evidence for nutritional interventions in ADHD is promising but preliminary. A comprehensive review of 54 studies concluded that while associations between specific nutrients and ADHD symptoms exist, the research doesn't yet support definitive dietary recommendations for managing ADHD (Pelsser et al., 2023). Nutrition is a complementary performance variable, not a replacement for medication, therapy, or coaching.
Conclusion
The ADHD athlete's nutrition challenge isn't a knowledge gap; it's a systems gap. You probably already know that protein matters, that omega-3s help, and that you should eat before training. The issue is that standard nutrition advice requires neurotypical executive function, and your brain doesn't operate that way.
Reframe nutrition as a training variable. Periodise your fuelling around your executive function capacity, not around an idealised meal plan you'll abandon by Wednesday. Start with Tier 1 defaults: the foods that require nothing from you on your worst day. Build from there when your brain allows it. And consider that external accountability, whether that's a coach, a structured programme, or a training partner, isn't a sign of weakness. It's a performance tool that elite athletes have always used.
Progress over perfection. System over willpower. Always.
If this resonated, I write about ADHD, performance, and the coaching strategies most people don't talk about in my newsletter.
Want to build a personalised fuelling system with accountability? Explore working with me →
Sources Referenced
Sogard, A.S. et al. (2026). "Nutrition for Youth Athletes with ADHD: What We Know and Practical Applications." Nutrients, 18(2), 282. https://pmc.ncbi.nlm.nih.gov/articles/PMC12845029/
Baik, J.H. (2021). Dopaminergic control of the feeding circuit. Endocrinology and Metabolism, 36(2), 229–239. https://doi.org/10.3803/EnM.2021.979; Wellman, P.J. (2005). Modulation of eating by central catecholamine systems. Current Drug Targets, 6(2), 191–199. https://doi.org/10.2174/1389450053174532
Clark, N. (2022/2025). "Can Diet Help Athletes Manage ADHD?" American College of Sports Medicine. https://acsm.org/diet-manage-adhd/
Pelsser, L.M. et al. (2023). "Nutrition in the Management of ADHD: A Review of Recent Research." Current Psychiatry Reports, PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC10444659/
Sheridan, C. et al. (2025). "A Closer Look at the Role of Nutrition in Children and Adults with ADHD and Neurodivergence." Frontiers in Psychiatry, PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC12343232/
CHADD (2023). "Nutrition and ADHD." Children and Adults with Attention-Deficit/Hyperactivity Disorder. https://chadd.org/about-adhd/nutrition-and-adhd/
ADDitude Magazine. "How Nutrition Harmonizes the ADHD Brain." https://www.additudemag.com/nutrition-harmonizes-adhd-brain/
ADHD-BED Integrated (2025). "The Impact of Nutrition on ADHD Symptoms: A Comprehensive Review." https://adhd.clinic/news-research/the-impact-of-nutrition-on-adhd-symptoms-a-comprehensive-review/